|
|
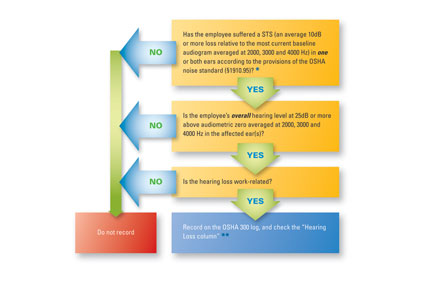
Note: In all cases, use the most current baseline to
determine recordability as you would to calculate an STS
under the hearing conservation provisions of the noise
standard (§1910.95). If an STS occurs in only one ear,
you may only revise the baseline audiogram for that ear.
* The audiogram may be adjusted for presbycusis
(aging) as set out in 1910.95.
** A separate hearing loss column on the OSHA 300
Log beginning in Calendar year 2004.
|
article examines noise-induced hearing loss as both an injury and illness, and looks at ways to use leading indicators to prevent occupational hearing loss.
Role of audiometry
Audiometry has been a key element in hearing conservation programs (HCP) since before the Hearing Conservation Amendment was enacted in 1981. Until recent emphasis on hearing loss prevention, results of audiometric testing were often the only measure of HCP effectiveness.
At a minimum, audiometric results must be evaluated to determine if a Standard Threshold Shift (STS) has occurred. An STS is defined as a shift in hearing from their baseline of an average of 10 decibels or more at the test frequencies of 2000, 3000 and 4000 hertz in either ear (after optional correction for aging). Following such shift, the OSHA regulation requires follow-up actions, including informing the worker and retesting. The OSHA recordability standard (2003) then requires that an STS resulting in a mild hearing impairment (worse than 25 dB) must be recorded on the OSHA 300 log.
Recordable hearing loss
Until 2004, occupational hearing loss was recorded as part of the “Other” category on the OSHA 300 Log. OSHA then added a hearing loss column to the 300 Log so the Bureau of Labor Statistics (BLS) could produce more reliable statistics on documented occupational hearing loss cases (66 FR 6005).
New recordability rules also redefined a recordable hearing loss from the previous definition of an average 25 dB change in hearing at 2000, 3000 and 4000 Hz as compared to the baseline audiogram to the current definition outlined above.
Professional organizations involved in hearing health applauded this change and more focus has been noted on hearing loss prevention efforts. However, change has not been without its consequences, including:
1) Possible under-reporting of hearing loss on the OSHA 300 Log
2) Pressure to determine hearing loss not work-related
3) Decrease in the hearing test as part of a wellness program
Under-reporting
In an audit published in 2009, the United States Government Accountability Office (GAO), found under-reporting on the OSHA 300 Log.1 The study cited evidence that worker and employer disincentives were primary factors in the inaccuracies of reporting illnesses and injuries. Another reason cited was a lack of understanding of OSHA’s record keeping requirements. One possible disincentive and a primary reason for these unintended consequences was that safety managers’ performance evaluations and bonuses were tied to having no recordable hearing loss.2
Pressure on practitioners
The GAO audit found that 53 percent of the health practitioners reported that they experienced pressure from company officials to downplay injuries or illnesses.
The OSHA regulation states: “You must use the rules in § 1904.5 to determine if the hearing loss is work-related. If an event or exposure in the work environment either caused or contributed to the hearing loss, or significantly aggravated a pre-existing hearing loss, you must consider the case to be work related.” (CFR 29, 1904.10, available at www.osha.gov).
Recordable STS can be “lined out or erased” if the hearing loss is not work-related. This provision for removing STS from the OSHA 300 Log is included so that hearing loss due to medical conditions such as otitis media (ear infection), otosclerosis, or Meniere’s disease would not be included with noise-induced hearing loss. However, the definition of hazardous noise is an important one. Some people, with very “tender ears” can suffer from noise-induced hearing loss at exposure levels as low as 80 dB depending on the length of time of the exposure. The length of most work shifts makes hearing loss unlikely at levels below 80 dB. If an employee is exposed at work to time-weighted average noise levels as low as 80 dB, it is difficult to prove that the noise at work didn’t contribute, thus making the resulting hearing loss recordable.
Fewer hearing tests in wellness programs
Many employers have ceased incorporating audiograms in company-wide wellness programs for non-noise-exposed employees for fear that they’d have to report any changes in hearing noted during wellness exams. If an employee has a hearing test as part of a company’s wellness program, but is not exposed to hazardous noise on the job, there should be no need to compare the results to a baseline. But even if the comparison is made, a decrease in hearing is noted, and is consistent with NIHL; the hearing loss may not be work-related and would therefore not be recordable.
Leading indicators
Employers should seek additional tools to help ensure their workers are not exposed to noise levels that can contribute to a recordable hearing loss. New technologies and tools train employees on positive hearing conservation behaviors and document such company efforts.
Earplug fit testing helps select the right earplug for the individual employee based on his or her noise exposure and provides feedback to train the employee to become skilled in properly fitting earplugs. Fit testing systems also provide additional documentation of training and product selection.3,4
In-ear dosimetry measures a collective dose of noise exposure throughout the work shift through the hearing protector whether or not it is worn. In-ear dosimetry’s metric — the employee’s percent of noise dose — is the ultimate leading indicator of noise-induced hearing loss and work-relatedness. It is possible to monitor the protected dose of noise to ensure levels are less than a 50 percent dose of hazardous noise throughout a work shift. In-ear dosimetry is ideal for employees who are showing a trend toward an STS or to train new employees on when and how to use hearing protection appropriately and effectively.5
|
References 1. “Workplace Safety and Health: Enhancing OSHA’s Record Audit Process Could Improve the Accuracy of Worker Injury and Illness Data” published in Oct 2009. www.gao.gov/products/GAO-10-10 2. “Confessions of a master manipulator” by Chris Morgan, ISHN (June 9, 2010). 3. Schulz, TY. Individual fit-testing of earplugs: A review of uses. Noise & Health, March, 2011, pp 152-162 4. Hager, LD. Fit-testing hearing protectors: An idea whose time has come. Noise & Health, March, 2011, pp. 147-151 5. Michael, K, Tougaw, and Wilkinson, R. Role of continuous monitoring in a hearing conservation program. Noise & Health, March, 2011, pp 195-199. |