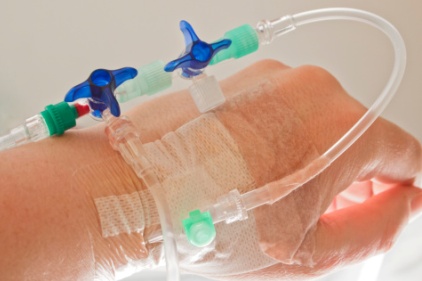
 A new National Institute for Occupational Safety and Health (NIOSH) study published online in the Journal of Occupational and Environmental Hygiene (JOEH) found that recommended safe handling practices for workers who administer antineoplastic drugs in healthcare settings are not always followed.
A new National Institute for Occupational Safety and Health (NIOSH) study published online in the Journal of Occupational and Environmental Hygiene (JOEH) found that recommended safe handling practices for workers who administer antineoplastic drugs in healthcare settings are not always followed.
Results are derived from the 2011 Health and Safety Practices Survey of Healthcare Workers, the largest federally-sponsored survey of healthcare workers in the U.S., which addresses safety and health practices relative to use of hazardous chemicals. This paper presents findings on current administrative and engineering control practices, personal protective equipment (PPE), and barriers to using recommended PPE during administration of antineoplastic drugs by nearly 2,100 oncology nurses and other healthcare personnel who completed a module addressing antineoplastic drug administration.
“Chemotherapy drugs save lives of cancer patients but also can result in adverse health outcomes in workers who are exposed to these drugs, including cancer, reproductive problems, and organ damage when recommended safe handling guidelines are not followed,” said NIOSH Director John Howard, MD. “Safeguarding healthcare workers from potential occupational hazards is an essential part of providing good jobs for these dedicated women and men, and furthering high-quality patient care.”
Findings suggest that best practices are not always used. Below are examples of practices that may increase exposure risk, expressed as percent of respondents:
- Not always wearing two pairs of chemotherapy gloves (80%) or not even a single pair (15%).
- Failure to always wear nonabsorbent gown with closed front and tight-fitting cuffs (42%).
- Intravenous (I.V.) tubing primed with antineoplastic drug instead of a non-drug containing liquid by the respondent (6%) or by the pharmacy department (12%).
- Potentially contaminated clothing taken home (12%).
- Spill or leak of antineoplastic drug during administration (12%).
- Lack of hazard awareness training (4%).
- Skin contact with antineoplastic drug (4%).
Despite the longstanding availability of authoritative safe handling guidelines (ASHP, NIOSH, ONS, OSHA), recommended exposure controls were not always used. According to NIOSH, this is highly noteworthy considering that there is no safe level of exposure to cancer-causing agents. Reported barriers to using PPE suggest that there is a perception that exposures are inconsequential or so rare that employers or workers feel PPE use is not justified.
The researchers conclude that better risk communication is needed to ensure that employers and employees are fully aware of the hazards and the availability of precautionary measures to minimize exposures. Commitment from all levels in the healthcare organization is essential to adequately protect workers from one of the most toxic classes of chemical agents used in healthcare.
Read the full study in the Journal of Occupational and Environmental Hygiene, which is published jointly by ACGIH® and AIHA. JOEH enhances the knowledge and practice of occupational and environmental hygiene and safety. It provides a written medium for the communication of ideas, methods, processes, and research in the areas of occupational, industrial, and environmental hygiene; exposure assessment; engineering controls; occupational and environmental epidemiology, medicine, and toxicology; ergonomics; and other related disciplines.